- Diabetes, Obesity and Metabolism
- Lower High-Density Lipoprotein Cholesterol Concentration Is Independently Associated with Greater Future Accumulation of Intra-Abdominal Fat
-
Sun Ok Song, You-Cheol Hwang, Han Uk Ryu, Steven E. Kahn, Donna L. Leonetti, Wilfred Y. Fujimoto, Edward J. Boyko
-
Endocrinol Metab. 2021;36(4):835-844. Published online August 27, 2021
-
DOI: https://doi.org/10.3803/EnM.2021.1130
-
-
4,409
View
-
120
Download
-
2
Web of Science
-
2
Crossref
-
 Abstract Abstract
 PDF PDF Supplementary Material Supplementary Material PubReader PubReader  ePub ePub
- Background
Both intra-abdominal fat (IAF) and high-density lipoprotein cholesterol (HDL-C) are known to be associated with cardiometabolic health. We evaluated whether the accumulation of computed tomography (CT)-measured IAF over 5 years was related to baseline HDL-C concentration in a prospective cohort study.
Methods
All participants were Japanese-Americans between the ages of 34 and 74 years. Plasma HDL-C concentration and CT measurements of IAF, abdominal subcutaneous fat (SCF), and thigh SCF cross-sectional areas were assessed at baseline and at 5-year follow-up visits.
Results
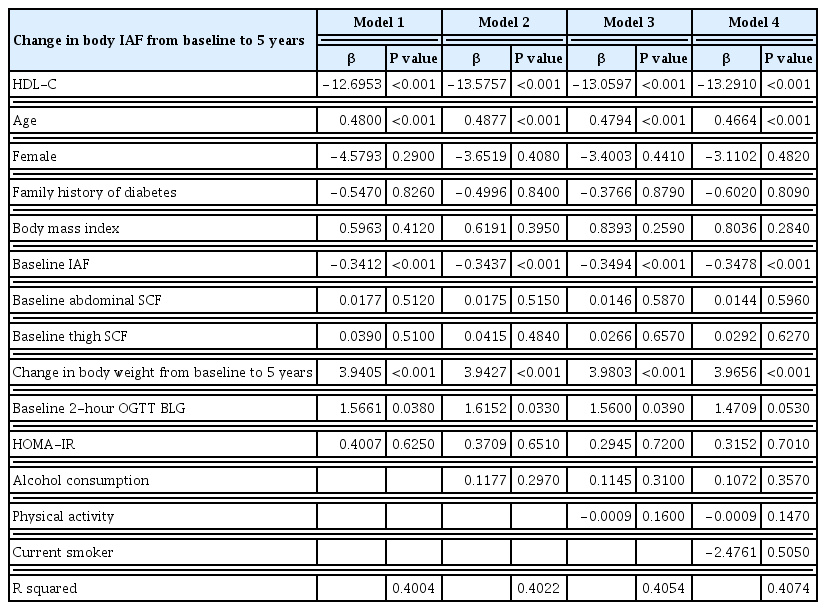
A total of 397 subjects without diabetes were included. The mean±standard deviation HDL-C concentration was 51.6±13.0 mg/dL in men and 66.0±17.0 mg/dL in women, and the IAF was 91.9±48.4 cm2 in men and 63.1±39.5 cm2 in women. The baseline plasma concentration of HDL-C was inversely associated with the change in IAF over 5 years using multivariable regression analysis with adjustment for age, sex, family history of diabetes, weight change over 5 years, and baseline measurements of body mass index, IAF, abdominal SCF, abdominal circumference, thigh SCF, and homeostatic model assessment for insulin resistance.
Conclusion
These results demonstrate that HDL-C concentration significantly predicts future accumulation of IAF over 5 years independent of age, sex, insulin sensitivity, and body composition in Japanese-American men and women without diabetes.
-
Citations
Citations to this article as recorded by  - Fenofibrate add-on to statin treatment is associated with low all-cause death and cardiovascular disease in the general population with high triglyceride levels
Kyung-Soo Kim, Sangmo Hong, Kyungdo Han, Cheol-Young Park
Metabolism.2022; 137: 155327. CrossRef - The associations between lipid profiles and visceral obesity among gastrointestinal cancer patients: a cross-sectional study
Bo Gao, Xiangrui Li, Wenqing Chen, Shu’an Wang, Jian He, Yu Liu, Chao Ding, Xiaotian Chen
Lipids in Health and Disease.2022;[Epub] CrossRef
- Clinical Study
- Clinical Outcomes of COVID-19 Patients with Type 2 Diabetes: A Population-Based Study in Korea
-
Ji Hong You, Sang Ah Lee, Sung-Youn Chun, Sun Ok Song, Byung-Wan Lee, Dae Jung Kim, Edward J. Boyko
-
Endocrinol Metab. 2020;35(4):901-908. Published online December 10, 2020
-
DOI: https://doi.org/10.3803/EnM.2020.787
-
-
6,866
View
-
233
Download
-
16
Web of Science
-
20
Crossref
-
 Abstract Abstract
 PDF PDF Supplementary Material Supplementary Material PubReader PubReader  ePub ePub
- Background
The aim of this study was to evaluate clinical outcomes in coronavirus disease 2019 (COVID-19) positive patients with type 2 diabetes compared to those without diabetes in Korea.
Methods
We extracted claims data for patients diagnosed with COVID-19 from the National Health Insurance Service database in Korea from January 20, 2020 to March 31, 2020. We followed up this cohort until death from COVID-19 or discharge from hospital.
Results
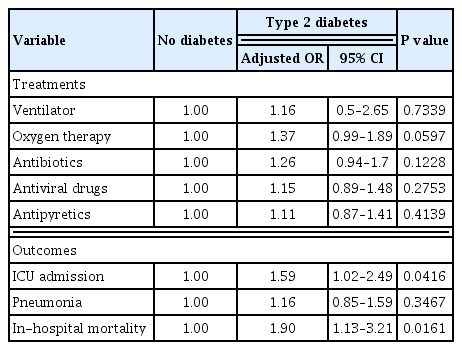
A total of 5,473 patients diagnosed with COVID-19 were analyzed, including 495 with type 2 diabetes and 4,978 without diabetes. Patients with type 2 diabetes were more likely to be treated in the intensive care unit (ICU) (P<0.0001). The incidence of inhospital mortality was higher in patients with type 2 diabetes (P<0.0001). After adjustment for age, sex, insurance status, and comorbidities, odds of ICU admission (adjusted odds ratio [OR], 1.59; 95% confidence interval [CI], 1.02 to 2.49; P=0.0416) and in-hospital mortality (adjusted OR, 1.90; 95% CI, 1.13 to 3.21; P=0.0161) among patients with COVID-19 infection were significantly higher in those with type 2 diabetes. However, there was no significant difference between patients with and without type 2 diabetes in ventilator, oxygen therapy, antibiotics, antiviral drugs, antipyretics, and the incidence of pneumonia after adjustment.
Conclusion
COVID-19 positive patients with type 2 diabetes had poorer clinical outcomes with higher risk of ICU admission and in-hospital mortality than those without diabetes. Therefore, medical providers need to consider this more serious clinical course when planning and delivering care to type 2 diabetes patients with COVID-19 infection.
-
Citations
Citations to this article as recorded by  - Reasons for Hospitalization Among Australians With Type 1 or Type 2 Diabetes and COVID-19
Dunya Tomic, Jonathan E. Shaw, Dianna J. Magliano
Canadian Journal of Diabetes.2024; 48(1): 53. CrossRef - Predictors of COVID-19 outcome in type 2 diabetes mellitus: a hospital-based study
Amira M. Elsayed, Mohamad S. Elsayed, Ahmed E. Mansour, Ahmed W. Mahedy, Eman M. Araby, Maha H. Morsy, Rasha O. Abd Elmoniem
The Egyptian Journal of Internal Medicine.2024;[Epub] CrossRef - Diabetes Mellitus and Pneumococcal Pneumonia
Catia Cilloniz, Antoni Torres
Diagnostics.2024; 14(8): 859. CrossRef - Risk for Newly Diagnosed Type 2 Diabetes Mellitus after COVID-19 among Korean Adults: A Nationwide Matched Cohort Study
Jong Han Choi, Kyoung Min Kim, Keeho Song, Gi Hyeon Seo
Endocrinology and Metabolism.2023; 38(2): 245. CrossRef - The Intersection of COVID-19 and Metabolic-Associated Fatty Liver Disease: An Overview of the Current Evidence
Mykhailo Buchynskyi, Iryna Kamyshna, Valentyn Oksenych, Nataliia Zavidniuk, Aleksandr Kamyshnyi
Viruses.2023; 15(5): 1072. CrossRef - Risk phenotypes of diabetes and association with COVID-19 severity and death: an update of a living systematic review and meta-analysis
Sabrina Schlesinger, Alexander Lang, Nikoletta Christodoulou, Philipp Linnerz, Kalliopi Pafili, Oliver Kuss, Christian Herder, Manuela Neuenschwander, Janett Barbaresko, Michael Roden
Diabetologia.2023; 66(8): 1395. CrossRef - Diabetes and deaths of COVID-19 patients: Systematic review of meta-analyses
Aakriti Garg, Mahesh Kumar Posa, Anoop Kumar
Health Sciences Review.2023; 7: 100099. CrossRef - Cardiometabolic Risk Factors and COVID-19 Outcomes in the Asia-Pacific Region: A Systematic Review, Meta-analysis and Meta-regression of 84,011 Patients
Ru Ying Fong, Annie Lee, Fei Gao, Jonathan Jiunn Liang Yap, Khung Keong Yeo
Journal of Asian Pacific Society of Cardiology.2023;[Epub] CrossRef - Pituitary Diseases and COVID-19 Outcomes in South Korea: A Nationwide Cohort Study
Jeonghoon Ha, Kyoung Min Kim, Dong-Jun Lim, Keeho Song, Gi Hyeon Seo
Journal of Clinical Medicine.2023; 12(14): 4799. CrossRef - Factors influencing the severity of COVID-19 course for patients with diabetes mellitus in tashkent: a retrospective cohort study
A. V. Alieva, A. A. Djalilov, F. A. Khaydarova, A. V. Alimov, D. Z. Khalilova, V. A. Talenova, N. U. Alimova, M. D. Aripova, A. S. Sadikova
Obesity and metabolism.2023; 20(2): 92. CrossRef - Genetic Predictors of Comorbid Course of COVID-19 and MAFLD: A Comprehensive Analysis
Mykhailo Buchynskyi, Valentyn Oksenych, Iryna Kamyshna, Sandor G. Vari, Aleksandr Kamyshnyi
Viruses.2023; 15(8): 1724. CrossRef - Anti-SARS-CoV-2 antibody levels predict outcome in COVID-19 patients with type 2 diabetes: a prospective cohort study
Sylvia Mink, Christoph H. Saely, Andreas Leiherer, Matthias Frick, Thomas Plattner, Heinz Drexel, Peter Fraunberger
Scientific Reports.2023;[Epub] CrossRef - Two years of SARS-CoV-2 infection (2019–2021): structural biology, vaccination, and current global situation
Waqar Ahmad, Khadija Shabbiri
The Egyptian Journal of Internal Medicine.2022;[Epub] CrossRef - Baseline haemoglobin A1c and the risk of COVID‐19 hospitalization among patients with diabetes in the INSIGHT Clinical Research Network
Jea Young Min, Nicholas Williams, Will Simmons, Samprit Banerjee, Fei Wang, Yongkang Zhang, April B. Reese, Alvin I. Mushlin, James H. Flory
Diabetic Medicine.2022;[Epub] CrossRef - The Role of Diabetes and Hyperglycemia on COVID-19 Infection Course—A Narrative Review
Evangelia Tzeravini, Eleftherios Stratigakos, Chris Siafarikas, Anastasios Tentolouris, Nikolaos Tentolouris
Frontiers in Clinical Diabetes and Healthcare.2022;[Epub] CrossRef - Impact of Type 2 Diabetes Mellitus on the Incidence and Outcomes of COVID-19 Needing Hospital Admission According to Sex: Retrospective Cohort Study Using Hospital Discharge Data in Spain, Year 2020
Jose M. de Miguel-Yanes, Rodrigo Jimenez-Garcia, Javier de Miguel-Diez, Valentin Hernández-Barrera, David Carabantes-Alarcon, Jose J. Zamorano-Leon, Ricardo Omaña-Palanco, Ana Lopez-de-Andres
Journal of Clinical Medicine.2022; 11(9): 2654. CrossRef - The burden and risks of emerging complications of diabetes mellitus
Dunya Tomic, Jonathan E. Shaw, Dianna J. Magliano
Nature Reviews Endocrinology.2022; 18(9): 525. CrossRef - A Comprehensive Analysis of Chinese, Japanese, Korean, US-PIMA Indian, and Trinidadian Screening Scores for Diabetes Risk Assessment and Prediction
Norma Latif Fitriyani, Muhammad Syafrudin, Siti Maghfirotul Ulyah, Ganjar Alfian, Syifa Latif Qolbiyani, Muhammad Anshari
Mathematics.2022; 10(21): 4027. CrossRef - New-Onset Diabetes Mellitus Presenting As Diabetic Ketoacidosis in Patients With COVID-19: A Case Series
Aysha Sarwani, Mahmood Al Saeed, Husain Taha, Rawdha M Al Fardan
Cureus.2021;[Epub] CrossRef - The management of type 2 diabetes before, during and after Covid-19 infection: what is the evidence?
Leszek Czupryniak, Dror Dicker, Roger Lehmann, Martin Prázný, Guntram Schernthaner
Cardiovascular Diabetology.2021;[Epub] CrossRef
- Clinical Study
- Apolipoprotein B Levels Predict Future Development of Hypertension Independent of Visceral Adiposity and Insulin Sensitivity
-
Seung Jin Han, Wilfred Y. Fujimoto, Steven E. Kahn, Donna L. Leonetti, Edward J. Boyko
-
Endocrinol Metab. 2020;35(2):351-358. Published online June 24, 2020
-
DOI: https://doi.org/10.3803/EnM.2020.35.2.351
-
-
5,822
View
-
130
Download
-
7
Web of Science
-
7
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader  ePub ePub
- Background
High plasma apolipoprotein B (apoB) levels have been shown to be associated with hypertension, central obesity, and insulin resistance in cross-sectional research. However, it is unclear whether apoB levels predict future hypertension independent of body composition and insulin sensitivity. Therefore, we prospectively investigated whether plasma apoB concentrations independently predicted the risk of hypertension in a cohort of Japanese Americans.
Methods
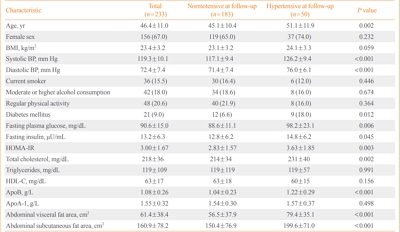
A total of 233 normotensive Japanese Americans (77 men, 156 women; mean age, 46.4±11.0 years) were followed over 10 years to monitor them for the development of hypertension. Fasting plasma concentrations of apoB, glucose, and insulin were measured at baseline. Insulin sensitivity was estimated using the homeostasis model assessment of insulin resistance (HOMA-IR). The abdominal visceral and subcutaneous fat areas were measured at baseline using computed tomography. Logistic regression analysis was used to estimate the association between apoB concentrations and the odds of incident hypertension.
Results
The 10-year cumulative incidence of hypertension was 21.5%. The baseline apoB level was found to be positively associated with the odds of incident hypertension over 10 years after adjustment for age, sex, body mass index, systolic blood pressure, abdominal visceral fat area, abdominal subcutaneous fat area, total plasma cholesterol concentration, diabetes status, and HOMA-IR at baseline (odds ratio and 95% confidence interval for a 1-standard deviation increase, 1.89 [1.06 to 3.37]; P=0.030).
Conclusion
Higher apoB concentrations predicted greater risks of future hypertension independent of abdominal visceral fat area and insulin sensitivity in Japanese Americans.
-
Citations
Citations to this article as recorded by  - Correlation between Central Obesity and Liver Function in Young Adults—A Cross-Sectional Study
John Alvin, Damodara Gowda KM
Journal of Health and Allied Sciences NU.2023; 13(02): 273. CrossRef - Serum amyloid A in children and adolescents: association with overweight and carotid intima-media thickness
Maria Vitória Mareschi Barbosa, João Carlos Pina Faria, Stephanie Ramos Coelho, Fernando Luiz Affonso Fonseca, Andrea Paula Kafejian Haddad, Fabíola Isabel Suano de Souza, Roseli Oselka Saccardo Sarni
einstein (São Paulo).2023;[Epub] CrossRef - The association of the apolipoprotein B/A1 ratio and the metabolic syndrome in children and adolescents: a systematic review and meta-analysis
Kayhan Dinpanah, Toba Kazemi, Sameep Shetty, Saeede Khosravi Bizhaem, Ali Fanoodi, Seyed Mohammad Riahi
Journal of Diabetes & Metabolic Disorders.2023;[Epub] CrossRef - Current Data and New Insights into the Genetic Factors of Atherogenic Dyslipidemia Associated with Metabolic Syndrome
Lăcramioara Ionela Butnariu, Eusebiu Vlad Gorduza, Elena Țarcă, Monica-Cristina Pânzaru, Setalia Popa, Simona Stoleriu, Vasile Valeriu Lupu, Ancuta Lupu, Elena Cojocaru, Laura Mihaela Trandafir, Ștefana Maria Moisă, Andreea Florea, Laura Stătescu, Minerva
Diagnostics.2023; 13(14): 2348. CrossRef - Sex-Based Differences and Risk Factors for Comorbid Nonalcoholic Fatty Liver Disease in Patients with Bipolar Disorder: A Cross-Sectional Retrospective Study
Ying Wang, Yiyi Liu, Xun Zhang, Qing Wu
Diabetes, Metabolic Syndrome and Obesity.2023; Volume 16: 3533. CrossRef - Apolipoprotein B Displays Superior Predictive Value Than Other Lipids for Long-Term Prognosis in Coronary Atherosclerosis Patients and Particular Subpopulations: A Retrospective Study
Chunyan Zhang, Jingwei Ni, Zhenyue Chen
Clinical Therapeutics.2022; 44(8): 1071. CrossRef - Genetics of Cholesterol-Related Genes in Metabolic Syndrome: A Review of Current Evidence
Sok Kuan Wong, Fitri Fareez Ramli, Adli Ali, Nurul ‘Izzah Ibrahim
Biomedicines.2022; 10(12): 3239. CrossRef
|